Know Your Headaches
Date
March 19, 2026
Credits

Date
March 19, 2026
Credits
Medical providers featured in this article
In Brief
{{cta-block}}
Most of us don’t give headaches much thought. We swallow a couple of pain relievers, sip some water and power through. But for millions ofAmericans, headaches aren’t an inconvenience—they’re a chronic condition that disrupts work, family obligations and quality of life.
“People often minimize headaches, but they can be profoundly disabling,” said Katrina Pasao, MD, a Cedars-Sinai headache specialist. “The good news is that we have more effective ways to diagnose and treat them than ever before.”
Head Pain Explained: Primary Versus Secondary Headaches
Headaches develop for many reasons, including stress, poor sleep, dehydration, illness, muscle tension and medication overuse.
“Some individuals are genetically predisposed to headaches and have increased sensitivity to common headache triggers compared to the general population,” said Pasao.
All headaches are associated with pain and discomfort in the head or face, but there are more than 100 different kinds, with varying symptoms and intensity.
A “primary headache” is when head pain is the main medical problem. A “secondary headache” happens as a result of another underlying condition. In rare cases, severe headache can signal a serious medical situation that requires immediate attention.
Understanding what’s behind your symptoms—and how different headache types behave—can help guide treatment and prevent pain from becoming a recurring problem.
Primary Headache Types
Most primary headaches fall into three main categories:
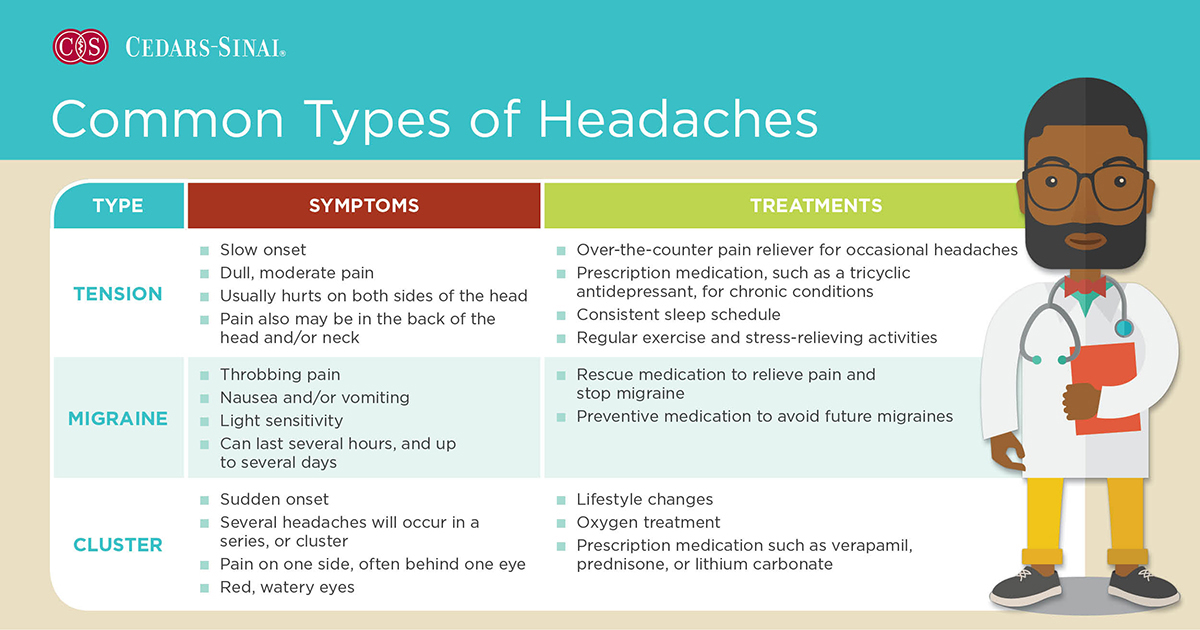
Tension headaches
The most common typeof headache, tension headaches often feel like a tight band wrapping around thehead or a dull ache behind the eyes. They’re frequently linked to stress, poorposture and muscle tension in the neck and shoulders.
What helps: Fortunately, most tension headaches respond to over-the-counter pain relievers, if they occur only occasionally. Chronic headaches may require prescription medication, along with good sleep hygiene, adequate hydration and regular meals, and relaxation techniques such as yoga, meditation or massage.
“Neck physical therapy, stretching and massage can make a dramatic difference for some patients,” said Pasao.
Migraine headaches
Migraines go far beyond typical head pain. They’re often throbbing, usually on one side of the head and frequently accompanied by nausea, vomiting and sensitivity to light, sound and smell. Some people experience visual changes or tingling sensations, known as aura, before pain begins.
“Migraines have a strong genetic component,” said Pasao. “They’re also influenced by irregular sleep patterns, hormones, diet and stress.”
Common migraine triggers include:
- Irregular sleep
- Dehydration
- Skipped meals
- Alcohol
- Certain foods, including aged cheeses and processed meats
- Hormonal fluctuations
What helps: Recognizing early warning signs can make a major difference. Subtle symptoms, such as fatigue, yawning, irritability or brain fog, may begin hours or even days before pain strikes. “The earlier you treat a migraine, the less intense the headache,” said Pasao.
Cluster headaches
Cluster headaches are far less common, but among the most painful conditions known in medicine. They cause piercing pain around one eye and often occur in predictable cycles lasting weeks or months. Patients may also experience eye redness and tearing, nasal congestion, drooping eyelids and intense restlessness.
“People with cluster headaches often can’t sit still because the pain is so severe,” said Pasao.
What helps: Treatment typically requires a specialized plan that may include oxygen therapy, injectable medications and preventive strategies.
There’s so much we can do for headaches—it doesn’t have to be debilitating. With sensible lifestyle strategies, careful tracking and the right treatment plan, most people find meaningful relief that lasts.”
A New Era in Headache Treatment
While it’s tempting to treat head pain with over-the-counter pain relievers, taking medications more than about 10 to 15 days per month can lead to medication-overuse headaches, also known as rebound headaches.
“If you’re relying on over-the-counter medications several times per week, it’s time to talk to a doctor,” said Pasao. “Headache care has advanced dramatically in recent years.”
In addition to medications that intercept a headache before it sets in, doctors have several options for headache care, including:
- Tricyclic anti-depressants, blood pressure medications, anti-seizure medications, SNRI antidepressants and triptans that have been proven effective against migraine.
- CGRP inhibitors, a new class of drugs that block specific pathways involved in migraine development.
- Botox injections, which have been shown to help curb headache frequency and intensity.
How Lifestyle Impacts Headache Frequency and Intensity
While medications play an important role, lifestyle habits often determine how frequently headaches strike. Before moving to prescription options, and even over-the-counter pain relievers, Pasao recommends addressing four essential pillars:
- Sleep: Poor or irregular sleep is one of the most powerful headache triggers. Maintain a consistent bedtime, limit screen use before sleep and address sleep disorders such as insomnia or sleep apnea to reduce headache frequency.
- Hydration: Dehydration is a frequent, and easily overlooked, trigger—even mild dehydration can worsen headache symptoms.Skipping meals can also provoke headaches by destabilizing blood sugar levels.
- Posture: Neck tension contributes to many tension-type headaches. Gentle stretching, targeted physical therapy and ergonomic adjustments at your desk can help relieve symptoms.
- Stress: Stress doesn’t just affect mood.It physically tightens muscles and disrupts sleep. Regular exercise, breathing techniques, yoga, massage and mindfulness practices can all help interrupt this cycle.
No matter which type of headache you have, keeping a headache diary or recording data in a tracking app can help identify patterns. In some cases, you may even intercept a headache before it fully develops.
Here’s what to track: When headaches occur, how long they last, pain severity, treatments and triggers (what you were eating, drinking or doing before the headache began).
When to Get Help for Head Pain
Most headaches resolve within a few hours to a day. If you have a headache for three days or longer, or a headache that won’t go away despite treatment, it’s important to seek medical attention.
Similarly, if you’re averaging more than four headache days each month, or headaches are interfering with work, family life or daily activities, make an appointment with your healthcare provider.
Red-flag symptoms that require immediate care include:
- Sudden loss of vision or consciousness
- Weakness, confusion or slurred speech
- Persistent vomiting
- Fever with stiff neck
- Headache lasting more than 72 hours
“There’s so much we can do for headaches—it doesn’t have to be debilitating,” said Pasao. “With sensible lifestyle strategies, careful tracking and the right treatment plan, most people find meaningful relief that lasts.”
Frequently Asked Questions
What are the most common triggers of headache?
The most common causes of headaches include stress, poor sleep, dehydration, skipped meals, muscle tension, illness and medication overuse. Identifying personal triggers can help prevent frequent headaches. Sometimes lifestyle changes and avoiding triggers may not be enough for individuals who are genetically predisposed to headaches. In these cases, medications can help decrease debilitating symptoms.
How long should a headache last?
Most headaches resolve within a few hours to a day. If a headache lasts longer than three days, returns quickly after treatment or doesn’t respond to medication, it’s time to seek medical care.
When is a headache considered severe or an emergency?
Seek immediate medical attention for a sudden, severe headache, loss of vision or consciousness, confusion, weakness, persistent vomiting, fever with stiff neck or a headache that lasts longer than 72 hours.
Can lifestyle changes really reduce headaches?
Yes. Improving sleep habits, staying hydrated, eating regular meals, managing stress and correcting posture can significantly reduce both headache frequency and intensity.
When should I see a doctor for frequent headaches?
If you have more than four headache days per month, rely on pain medication several times a week or find that headaches interfere with daily life, schedule an appointment with your healthcare provider.